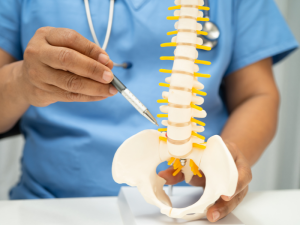
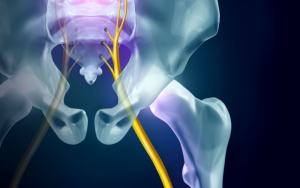
Trauma and chronic pain often coexist because sometimes, people with persistent pain also have an untreated or complex trauma history. Pain is our body’s danger detection system, making the body and mind more sensitive, and trauma changes the brain.
If someone has a history of trauma, their brain will strengthen their body’s sensory messages to protect and keep them safe. The brain becomes hypervigilance in scanning a person’s internal and external environment, looking for potential danger, often overreacting in self-protection mode with minimal stimulus. For example, most times, a tap on the shoulder is not dangerous, but if someone has experienced trauma, they might have a strong startle response and ‘jump out of their skin.’ Does this sound familiar? Hypervigilance is one symptom of Post Traumatic Stress Disorder (PTSD).

Chronic pain can most cases, be avoided by
- Validating and managing any untreated trauma.
- Addressing anxiety and stress
- Ensuring those affected have a social support network. According to neuroscience, social medicine is genuine.
It is essential to communicate that recovery from persistent pain is rarely straightforward. It’s complex and complicated because it involves our brain, body, environment, and, importantly, all our previous experiences and learnt behaviour from childhood all jumbled together like a puzzle. We need to put the pieces back to make sense of our situation. What’s critical is that a multilayered approach seems to work best; for example, distraction strategies can help, but that’s just one piece of this pain puzzle. More than distraction is required, and while addressing our emotions and changing thoughts or reducing anxiety is beneficial, this is not enough.
Have you noticed when you are distracted or deeply absorbed in an activity, you can forget about the pain, even if that is only a brief experience? That is not magic; it’s neuroscience (brain) science. Like most healthcare professionals, I was taught little about persistent/chronic pain during my long undergraduate training; this knowledge was gained via extensive post-graduate education and continuation professional development (CPD) with some leading pain experts worldwide. This knowledge transformed my life personally and professionally.
 If people want to change their pain, they need to know that pain that persists is rarely a purely medical or biological problem. It’s a biopsychosocial problem involving biological, psychological, and social factors and their complex interactions in understanding health, illness, and healthcare delivery. These exist along a continuum, and. I spend much of my time battling against the stigma caused by the psychological aspect of pain that results in so much self and societal stigma.
If people want to change their pain, they need to know that pain that persists is rarely a purely medical or biological problem. It’s a biopsychosocial problem involving biological, psychological, and social factors and their complex interactions in understanding health, illness, and healthcare delivery. These exist along a continuum, and. I spend much of my time battling against the stigma caused by the psychological aspect of pain that results in so much self and societal stigma.
By the way, this isn’t just my opinion; it’s current thinking in neuroscience. Our emotions and thoughts affect our bodies; consider how stress affects our bodies, tight neck and shoulders, clenched jaw, grinding teeth and churning stomach. A multidisciplinary biopsychosocial approach is needed to support those with persistent pain. For the record, I’m not saying bypass your doctor; your need to rule out the red flags, the rare and sinister stuff, check for tissue damage, system dysfunction, inflammation, nutritional deficiencies, or get pain medications. However, in most cases, know there is no quick fix for chronic pain, but the simple stuff works best; movement/exercise light and sleep are critical considerations. It’s always better to leave the risky interventions as the resort last.